Semana 11 Nutrición 10/10/2022
Supportive Nutrition in Healthcare
In this section, the instructor introduces the concept of supportive nutrition in healthcare, emphasizing its role in ensuring adequate energy and nutrient intake for patients undergoing medical procedures.
Supportive Nutrition Definition and Purpose
- Supportive nutrition comprises procedures that guarantee proper energy and nutrient consumption during diagnostic or therapeutic procedures.
- The goal of supportive nutrition is to maintain a patient's nutritional status, especially when undergoing diagnostic or therapeutic processes.
- It aims to restore or support the patient's nutritional state while hospitalized and undergoing medical tests.
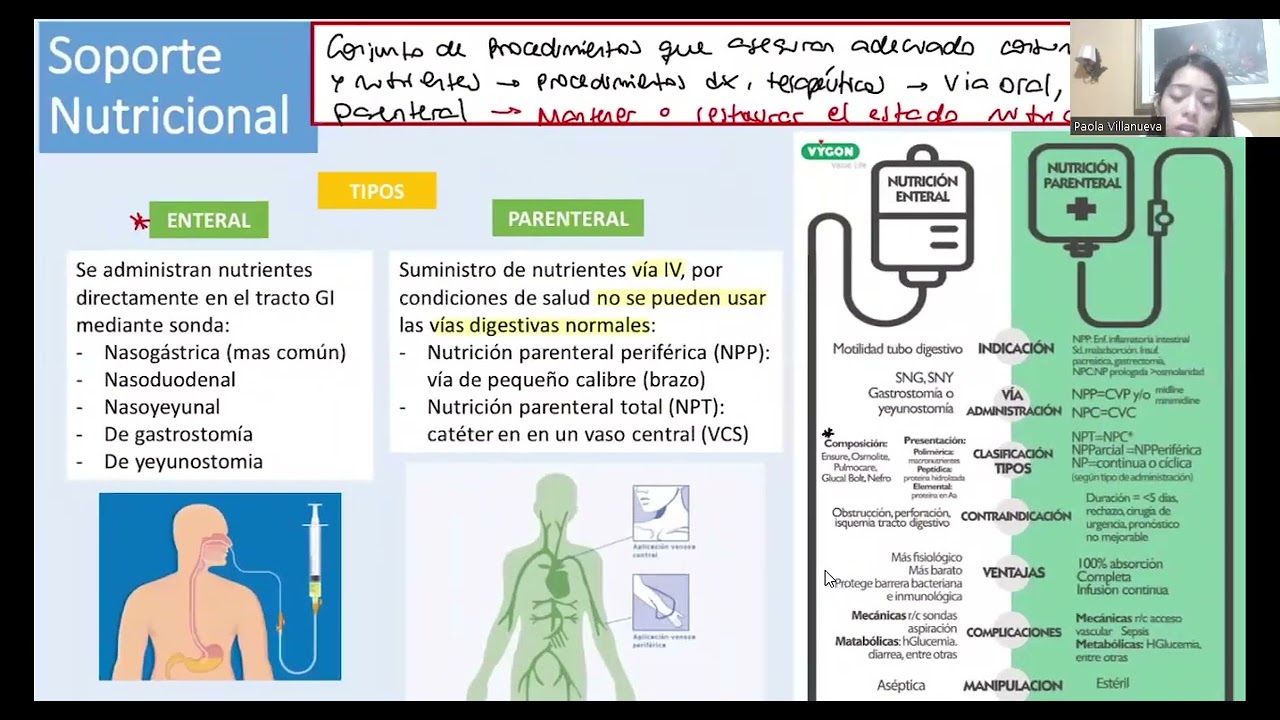
Enteral vs. Parenteral Nutrition
- Enteral nutrition involves administering nutrients directly into the gastrointestinal tract, typically through a nasogastric tube, promoting physiological absorption.
- Parenteral nutrition delivers nutrients intravenously when enteral feeding is not feasible, ensuring complete nutrient absorption but with larger calibre veins required.
Indications and Formulas
- Differentiate between enteral and parenteral nutrition based on patient conditions like mobile digestive system for enteral feeding and specific diseases for parenteral feeding.
- Various formulas such as Ensure, Osmolight, Pulmocare are used for enteral feeding, each tailored to different nutritional needs.
Contraindications and Advantages
- Contraindications for enteral feeding include obstructions or perforations in the gastrointestinal tract, while parenteral feeding may be preferred for certain conditions or surgeries.
Nutritional Support in Hospitalized Patients
The speaker discusses the potential complications and considerations related to nutritional support for hospitalized patients, emphasizing the importance of understanding when to provide such support based on various medical conditions.
Complications and Considerations for Nutritional Support
- Certain areas can be damaged by waves, leading to metabolic complications. For instance, Glucerna can cause diarrhea in some patients.
- Nutritional support is essential when there are gastrointestinal disturbances like obstruction or inflammatory conditions such as pancreatitis or Crohn's disease.
- Neurological issues like Alzheimer's or critical conditions where patients cannot feed themselves necessitate nutritional support to prevent complications like aspiration pneumonia.
- Psychiatric disorders such as anorexia or bulimia may also require nutritional support, especially in critically ill patients who cannot eat orally.
Impact of Malnutrition in Hospitalized Patients
The prevalence of malnutrition among hospitalized patients is discussed along with its implications on immune response, healing processes, and overall patient outcomes.
Consequences of Malnutrition
- Approximately 30% to 50% of hospitalized patients may experience malnutrition, affecting their immune response and delaying recovery.
- Malnourished patients exhibit poor immunological responses, leading to prolonged hospital stays, ventilator dependency, delayed wound healing, and increased mortality rates.
Enteral Nutrition Indications and Contradictions
The speaker elaborates on the indications and contraindications for enteral nutrition in patients who are unable to consume food orally due to various medical conditions.
Enteral Nutrition Guidelines
- Enteral nutrition is recommended for patients with neurological issues causing swallowing difficulties or those at risk of aspiration due to sedation or specific diseases like Alzheimer's.
- Patients with chronic illnesses like cancer or COPD who struggle with oral intake may benefit from enteral nutrition. It is also suitable for those unable to maintain adequate oral nutrition for more than 5 to 7 days.
Contraindications for Enteral Nutrition
The speaker outlines scenarios where enteral nutrition should be avoided due to potential risks or inefficacy in certain patient populations.
Situations Contradicting Enteral Nutrition
Gastrointestinal Support and Nutritional Routes
In this section, the discussion revolves around gastrointestinal support options and the criteria for deciding on enteral nutritional routes based on short-term and long-term needs.
Gastrointestinal Support Options
- Short-term enteral support (less than 3-4 weeks) commonly involves nasogastric tubes.
- Nasogastric tubes are preferred when there is no risk of aspiration or gastric issues.
- For long-term enteral support (more than four weeks), enterostomy is typically utilized.
Enteral vs. Parenteral Nutrition
- Parenteral nutrition is considered when the gastrointestinal tract is non-functional or inaccessible, such as in short bowel syndrome or gastrointestinal fistulas.
- Peripheral and central routes are chosen based on the duration of support needed and the patient's metabolic status.
Choosing Between Peripheral and Central Routes
- Peripheral route is preferred for support lasting less than 5-7 days, while central route is favored for longer durations or in hypermetabolic patients.
- Central lines are used for prolonged support in malnourished or at-risk patients.
Nutritional Support Indications and Considerations
This segment covers indications for different nutritional routes, emphasizing the importance of maintaining or restoring a patient's nutritional status through enteral or parenteral means.
Enteral vs. Parenteral Indications
- Enteral nutrition is physiologically preferable but may not always be feasible due to various conditions like gastrointestinal alterations, neurological issues, psychiatric problems, critical illness, or malnutrition.
Specific Considerations
- Desnutridos patients may require central venous access for parenteral nutrition due to increased nutrient requirements.
Metabolic Status and Nutritional Requirements Estimation
The discussion shifts towards estimating caloric requirements based on metabolic status to tailor appropriate nutritional interventions effectively.
Metabolic Status Consideration
Understanding Metabolic Patients and Nutritional Support
In this section, the speaker discusses metabolic patients and their nutritional requirements post-surgery, comparing them to non-operated patients. Different types of metabolic patients are highlighted, such as burn victims and polytrauma cases.
Metabolic Patients and Nutrient Requirements
- Post-surgery patients require more nutrients to return to their pre-surgery state.
- Metabolic patients like burn victims rapidly deplete nutrients and need higher quantities compared to regular individuals.
- Non-hypermetabolic patients, such as those with appendicitis, do not require parenteral support post-operation.
Nutrition Support Methods and Patient Care
This part delves into nutrition support methods for different patient categories, emphasizing the use of parenteral nutrition in certain cases. The discussion also touches on central vs. peripheral access for nutrient administration.
Parenteral Nutrition and Access Sites
- Some patients receive basic parenteral nutrition initially post-operation.
- Central access sites like subclavian veins are commonly used for parenteral nutrition over peripheral sites.
Criteria for Nutritional Support Methods
Criteria for selecting between enteral and parenteral nutrition methods are outlined here. The speaker explains the distinctions between central and peripheral access in nutritional care.
Criteria for Nutritional Support Selection
- Understanding the differences between enteral and parenteral nutrition is crucial for maintaining or restoring a patient's nutritional status.
- Specific considerations like fluid restrictions are essential when using central access for parenteral nutrition.
Indications for Enteral Nutrition Support
Indications for utilizing nasogastric feeding tubes in enteral nutrition support are discussed here. The importance of proper criteria selection is emphasized.
Nasogastric Feeding Criteria
- Nasogastric feeding tubes are suitable when enteral nutrition needs extend beyond three to four weeks.
- Exclusion criteria include a body mass index below 18.5 when considering nutritional support methods.