Leishmania
Leishmania: Understanding the Parasite and Its Impact
Introduction to Leishmania
- The study of microbiology must consider microorganisms that can cause multi-organ damage, particularly focusing on Leishmania due to its significant impact on medium and long-term prognosis.
- Leishmania is a unicellular or multicellular parasite that lives at the expense of its host, primarily humans, leading to a disease known as leishmaniasis.
Characteristics of Leishmania
- This protozoan parasite thrives in warm and humid climates, predominantly found in South America and Mediterranean countries.
- As an intracellular parasite, it invades human cells for reproduction and metabolism; its presence triggers immune reactions that manifest as symptoms of leishmaniasis.
Transmission and Vectors
- Humans are incidental hosts; primary hosts include rodents, marsupials, and wild canids.
- The transmission vector is the phlebotomine sandfly (Lutzomyia), which spreads the disease through bites rather than direct contact with infected animals.
Incubation Period and Symptoms
- The incubation period for leishmaniasis varies significantly from weeks to years after infection, complicating diagnosis.
- Besides skin lesions from bites, other affected areas include the nose, mouth, throat, liver, and spleen; individuals with compromised immune systems are more severely impacted.
Morphology and Life Cycle
- The morphology of Lutzomyia allows it to transmit Leishmania by feeding on infected blood; parasites move from the mosquito's digestive system to its salivary glands.
- When biting a human host, the mosquito regurgitates promastigotes into the bloodstream where they transform into amastigotes within human cells.
Variants of Leishmania
- Different forms of Leishmania exist based on their manifestations in humans: visceral leishmaniasis (Donovan type), cutaneous types (e.g., Mexican variant), and mucosal types affecting nasal passages (Amazonian variant).
Conclusion: Life Cycle Dynamics
Understanding Leishmania Transmission and Effects
Mechanism of Infection
- Once plastic enters the body, macrophages quickly attempt to engulf it. However, the parasite has morphological and metabolic characteristics that prevent its destruction.
- The parasite transforms from a form carried by mosquitoes (promastigote) to a replicating form (amastigote) once inside humans, leading to continuous replication within macrophages.
- As macrophages burst due to overwhelming numbers of parasites, they release more parasites into the bloodstream, which are then consumed by new macrophages in an ongoing cycle of infection.
Transmission Pathways
- The primary transmission route is through mosquito bites; however, congenital transmission can occur if infected mothers pass the parasite to their offspring during pregnancy.
- While leishmaniasis does not cause congenital malformations, it can lead to severe complications such as fetal death or growth restrictions.
Immune Response and Inflammation
- The immune system responds to the presence of amastigotes with inflammation; this reaction can cause significant damage over time.
- Symptoms may take weeks or months to manifest as the body reacts to the infection with characteristic inflammatory responses.
Clinical Manifestations
- One severe manifestation is visceral leishmaniasis (kala azar), where parasites spread through blood circulation affecting various organs.
- Infected individuals may exhibit symptoms like pallor due to anemia, systemic fever in response to infection, and rapid weight loss.
Organ-Specific Effects
- The spleen becomes enlarged (splenomegaly), leading to pancytopenia—decreased levels of red blood cells (anemia), white blood cells (leukopenia), and platelets (thrombocytopenia).
- Liver involvement results in decreased production of important proteins like albumin and gamma globulin, increasing susceptibility to infections while causing bilirubin accumulation that leads to toxicity.
Additional Complications
- Lymph nodes may also be affected by amastigotes causing swelling, pain, ulceration, and secondary bacterial infections.
- Bone marrow disruption occurs due to parasitic presence affecting red blood cell production further exacerbating anemia and related complications.
Leishmaniasis: Understanding the Risks and Prognosis
Overview of Leishmaniasis and Its Complications
- The risk of superinfection with Staphylococcus aureus is always present in leishmaniasis, particularly in its most severe form, which can lead to multi-organ failure and often results in death.
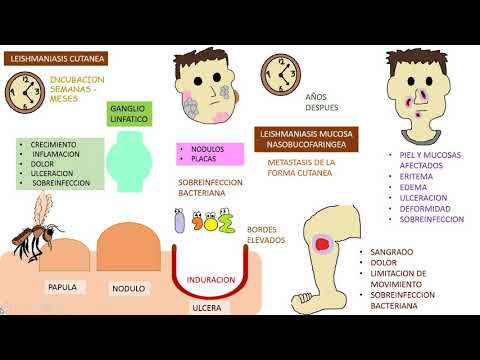
- Cutaneous leishmaniasis has an incubation period that can last weeks or months; symptoms may include papules, nodules, and ulcerations at the mosquito bite site.
- Ulcers characteristic of leishmaniasis can appear anywhere on the body, causing pain, bleeding, limited movement, and local lymph node involvement with inflammation and potential superinfection.
- Lesions may develop into dark gray nodules or plaques that are also susceptible to infection; Staphylococcus aureus poses a constant threat if given the opportunity.
- Chronic cutaneous leishmaniasis can evolve into mucosal leishmaniasis affecting the nose, mouth, and throat if untreated or improperly treated.
Symptoms and Diagnosis
- Mucosal lesions can cause deformities such as nasal septum damage leading to unpleasant appearances and internal mucosa exposure resulting in bleeding and pain.
- Clinical diagnosis relies heavily on patient history including risk factors like endemic areas or prior organ transplants; early detection is crucial for effective treatment.
- Diagnostic methods include microscopy for parasite identification, molecular techniques for DNA detection, antibody searches against parasite components, and biopsy cultures from lesions.
- Differential diagnosis is essential as not all skin lesions indicate leishmaniasis; other pathological entities must be considered before concluding a diagnosis.
Treatment Approaches
- Treatment plans should be individualized based on patient comorbidities and specific forms of leishmania; monitoring is necessary as treatment duration may extend from weeks to months with partial cures possible.
- Prevention strategies focus on mosquito control and identifying cases early to prevent disease spread.
Key Points for Clinical Practice
- Important exam points include understanding infective forms in insects versus humans (amastigote), vector transmission by phlebotomine sandflies (Lutzomyia), with visceral leishmaniasis being the most aggressive form associated with poor prognosis (Kala-Azar).
- Giemsa or Romanowsky staining is recommended for protozoan identification in tissue biopsies; specialized laboratory cultures are required for growing Leishmania species effectively.
- The incubation period varies significantly from months to years; awareness of endemic regions is vital when diagnosing suspected cases of leishmaniasis.
Conclusion on Leishmania Types