SINDROME DE HELLP
Medical Condition: HELLP Syndrome
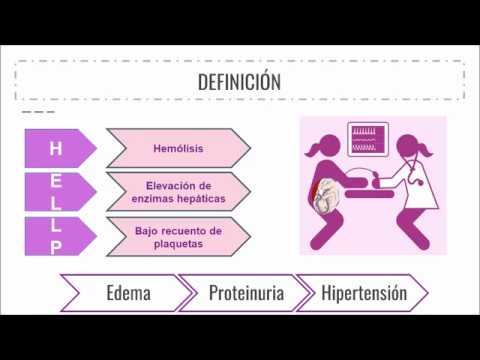
The discussion delves into HELLP syndrome, a severe form of preeclampsia occurring in late pregnancy or postpartum. It is characterized by hemolysis, elevated liver enzymes, and low platelet count.
Mechanism of HELLP Syndrome
- HELLP syndrome is considered a unique form of pregnancy-induced hypertension requiring pregnancy termination. The exact biological alteration mechanism is not fully understood but is believed to be related to severe placental damage.
- In normal pregnancy, alterations in the arteries supplying the placenta lead to inadequate immune tolerance and incomplete arterial transformation, potentially causing placental dysfunction and oxidative stress.
Clinical Manifestations and Diagnosis
- Placental abnormalities can result in endothelial injury, decreased nitric oxide production, leading to hypertension, proteinuria, edema, thrombocytopenia, and hepatic capsule distension.
- Diagnosis involves identifying hypertensive disorders like preeclampsia/eclampsia followed by the diagnostic triad: hemolysis, thrombocytopenia, elevated liver enzymes (especially lactate dehydrogenase).
Differential Diagnosis and Treatment
- Differential diagnoses include fatty liver of pregnancy and various thrombotic disorders. Immediate hospitalization for thorough evaluation is crucial due to rapid maternal-fetal deterioration potential.
- Treatment involves strict blood pressure control to prevent complications like cerebral hemorrhage. Prompt delivery is essential; corticosteroids may be administered for fetal lung maturation if preterm labor risk exists.
Laboratory Tests and Management
This segment focuses on laboratory investigations required for diagnosing HELLP syndrome and outlines management strategies for optimal patient care.
Laboratory Investigations
- Comprehensive lab tests are vital for assessing hepatic function (enzymes), renal function (creatinine), coagulation status (PTT), among others. These tests aid in confirming the diagnosis within 12-24 hours.
Management Strategies
- Hospitalization allows close monitoring as these patients' conditions can deteriorate rapidly. Blood pressure control with antihypertensives like hydralazine or beta-blockers is crucial.
- Fluid-electrolyte balance must be carefully maintained to avoid vasoconstriction-related organ damage. Early delivery remains the most effective treatment beyond 34 weeks gestation or with severe symptoms.
New Section
In this section, the speaker discusses the evaluation of fetal conditions through various tests and tools, emphasizing the importance of monitoring fetuses with hypertensive disorders during pregnancy.
Evaluation of Fetal Conditions
- Doppler ultrasound is crucial for monitoring fetuses with hypertensive disorders during pregnancy.
- Tests such as non-stress testing, contraction stress testing, and fetal biophysical profile are essential for evaluating fetal conditions.
- Signs and symptoms of complications include hypertension leading to headaches, blurred vision, localized pain in the right hypochondrium and epigastric region, nausea, vomiting, decreased fetal heart rate, platelet count reduction, decreased hemoglobin levels, increased liver enzymes and bilirubin levels.
New Section
This section delves into interventions related to monitoring vital signs in pregnant individuals with hypertensive disorders.
Monitoring Vital Signs
- It is crucial to monitor blood pressure before and after administering antihypertensive medications to assess the severity of hypertension accurately.
- Nursing interventions focus on identifying risks such as liver function deterioration in patients with HELLP syndrome.
New Section
The discussion shifts towards managing complications related to liver function in pregnant individuals with hypertensive disorders.
Managing Liver Function Complications
- Interventions involve monitoring for signs of hemorrhage due to potential liver rupture during or after childbirth.
- Coagulation studies should be conducted alongside controlling vital signs and administering blood products if necessary to address liver function issues effectively.
New Section
This part focuses on fluid management strategies and assessing hemodynamic risks in pregnant individuals with hypertensive disorders.
Fluid Management and Hemodynamic Assessment
- Monitoring fluid balance is essential by evaluating hemodynamic risks and edema extent while tracking vital signs and fluid intake/output.
- Assessing proteinuria presence aids in determining renal health status alongside other vital sign assessments for comprehensive care.