II) 8. Indicadores de calidad para enfermería (INDICAS)
Indicators of Quality and Safety in Nursing Care
Overview of the System
- The topic covers quality and safety indicators in nursing care, part of a strategy by the health department.
- The system allows monitoring and comparison of quality indicators across health services nationwide.
Types of Indicators
- There are indicators for primary care units, hospitals, medical personnel, and user treatment.
- Specific nursing indicators aim to ensure quality and safety in medical attention throughout the country.
Focus on Nursing Indicators
- Six specific nursing indicators are monitored at the second level of care.
- First three focus on medication administration, patient dignity by nurses, highlighting barriers to safety.
Safety Indicators in Patient Care
Key Safety Measures
- Three additional indicators address patient safety: fall prevention, pressure ulcer prevention, urinary tract infection prevention.
Sample Size Determination
- Sample size for applying these indicators is determined quarterly; not all patients are included.
Implementation Process
Data Collection Strategy
- Establishes how many patients will be surveyed each month/week based on previous quarter data.
High-Risk Patient Identification
- Focuses on high-risk patients for falls or pressure injuries to determine sample size effectively.
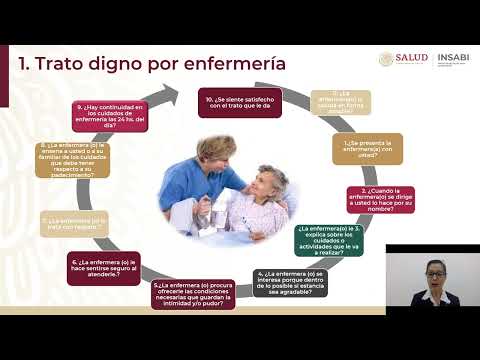
Dignified Treatment Indicator
Assessment Criteria
- The first indicator assesses dignified treatment through a specific form filled by nursing management during visits.
Patient Interaction Standards
Importance of Patient Interaction
- Nurses must address patients directly and explain essential actions to ensure understanding.
- Clear communication helps alleviate patient fears and ensures a pleasant hospital stay through kindness and respect.
- Nurses should maintain patient privacy during procedures by closing doors or curtains.
Ensuring Patient Comfort and Safety
- Nurses create a sense of security by explaining procedures, treating patients with respect, and using their names.
- Education for patients and families about care post-discharge is crucial to prevent confusion regarding medications.
- Continuity in nursing care is vital for effective treatment across shifts, ensuring comprehensive patient evaluations.
Evaluating Patient Satisfaction
- Direct questions to patients help assess their satisfaction with the care received from nursing staff.
- Friendly greetings upon introduction and departure are essential for establishing rapport with patients.
- Meeting 95% of established criteria indicates that nurses provide dignified treatment.
Infection Control Measures
- Proper management of infusion therapy reduces infection risks associated with healthcare settings.
- Seven key actions by nursing staff are necessary to prevent nosocomial infections related to intravenous therapy.
Documentation Standards in Nursing Care
- Accurate documentation includes patient details, service period, and specifics about the administered solution.
- Solutions must be changed every 24 hours; failure to do so can lead to complications or errors in treatment.
Guidelines for Venous Catheterization
- Use hypertonic solutions or parenteral nutrition; change equipment every 24 hours and label with installation date and time.
- Ensure the catheter is free of residues to prevent infections; check for compatibility of medications and solutions.
- Immediate changes are necessary if blood residues are found in the equipment, as this can lead to infection.
Monitoring Catheter Condition
- Assess peripheral catheter function through nursing records; report any pain or issues at the insertion site.
- Ensure catheters are securely installed and clean; avoid common mistakes in placement that could lead to complications.
- Maintain visibility of the insertion site using transparent dressings to monitor cleanliness.
Closed Circuit Solutions
- Use a closed circuit for parenteral solutions to minimize infection risk; ensure all connections are secure.
- Limit manipulation of the circuit during use, adhering strictly to safety protocols.
- Compliance with seven criteria reduces infection risks associated with peripheral catheters.
Medication Administration Protocol
- Verify patient data against medical orders before administering oral medications; ensure accuracy in medication delivery.
- Confirm medication name and presentation match medical indications to avoid errors during administration.
Medication Administration and Patient Safety
- Medication administration must adhere to official schedules and be recorded in the nursing clinical record.
- Inform patients about the medication being administered, ensuring they understand the procedure for their safety.
- Nurses should verify that patients actually ingest medications, especially during night shifts when patients may be asleep.
Ensuring Correct Medication Intake
- Presence of nursing staff is crucial when patients take medications to ensure proper administration.
- It’s important to document any alternate medications given according to established formats.
- Confirm that oral medications are fully ingested before recording them as administered.
Preventing Patient Falls
- Implement actions to prevent falls among hospitalized patients, focusing on risk factors.
- Utilize a checklist with seven criteria aimed at reducing fall risks in medical units.
- Assess patient fall risk using a scale and create personalized care plans based on identified risks.
Assessing Fall Risk Factors
- Evaluate previous falls, medication effects, sensory deficits, and mental state of the patient.
- Use scoring from the assessment scale to determine if a patient is at high, medium, or low risk for falls.
- Tailor interventions based on specific criteria from the fall risk assessment scale.
Utilizing Resources for Patient Safety
- Leverage available resources and equipment to enhance patient safety regarding fall prevention.
- Educate patients and families about fall risks and necessary precautions during hospital stays.
Utilization of Medical Equipment
- Importance of explaining the use of medical equipment like bed rails and crutches to patients and families.
- Nursing interventions must be re-evaluated based on patient condition at the start of each shift or when health status changes.
- Documenting any falls during care is crucial as it represents an adverse event.
Prevention of Pressure Ulcers
- Definition: Actions by nursing staff to prevent pressure ulcers in hospitalized patients.
- Increased incidence of pressure ulcers noted during COVID due to immobility among hospitalized patients.
- High rates observed in bedridden patients, emphasizing the need for proper care protocols.
Risk Assessment Criteria
- Six criteria established for assessing risk factors for pressure ulcers in patients.
- First criterion involves evaluating risk factors using a standardized scale (Braden Scale).
- Establishing a care plan based on identified risks is essential for effective patient management.
Patient and Family Education
- Educating patients and families about preventing pressure ulcers is vital, especially for those who will remain bedridden.
- Continuous re-evaluation of nursing interventions according to patient status helps mitigate risks effectively.
Braden Scale Overview
- The Braden Scale assesses sensory perception, moisture exposure, mobility, nutrition, friction, and shear risk factors.
- Scoring from 1 to 4 provides a risk level indicating potential for developing pressure ulcers.
Identifying Risks in Clinical Settings
- Lower scores indicate higher risk; thus, monitoring is critical in hospital settings.
Risk Management in Patient Care
- Discusses the use of a rotation clock to manage high-risk patients and prevent pressure injuries.
- Emphasizes adherence to guidelines for patient positioning regardless of diagnosis.
- Introduces urinary tract infection prevention measures for patients with indwelling catheters.
Key Indicators for Catheter Care
- Importance of keeping the collection bag below bladder level to prevent backflow and infections.
- Ensures catheter is secured according to patient's sex to avoid injury.
- Highlights the need for proper identification on catheters, including installation date and personnel details.
Maintaining Catheter Connection
- Stresses that drainage systems must remain connected to prevent infection risks.
- Encourages regular monitoring and documentation of catheter function and drainage system integrity.
- Advises on checking for kinks or obstructions in the catheter circuit.
Monitoring Catheter Duration
- Notes the importance of documenting days a catheter is in place as per medical prescriptions.
- Calls attention to recognizing signs of urinary tract infections, which are often overlooked by nursing staff.
- Lists symptoms such as changes in urine color, fever, or suprapubic pain that indicate potential infections.
Hygiene Practices for Patients with Catheters
- Recommends daily genital hygiene using soap and water to reduce infection risk.
- Emphasizes thorough cleaning techniques from pubis to catheter insertion site.
Importance of Avoiding Risks in Patient Care
- Focus on preventing attraction from the catheter to avoid patient harm and minimize risks associated with urinary catheters.
Evaluating Quality Indicators in Nursing
- Assessing indicators helps understand compliance with safety quality in nursing care.
- Nurses must be aware of actions required for each patient based on six key indicators.
Understanding Evaluation Criteria for Nursing Staff
- It's crucial for nursing staff to know the criteria used by management during evaluations.
- Awareness of these criteria allows nurses to meet compliance percentages effectively.
Standards and Documentation in Nursing Care
- The goal is to achieve 100% compliance with established quality indicators.