GMT20260126 221607 Recording 1366x768
Introduction to Diabetes in Geriatrics
Opening Remarks
- The session begins with a greeting and an invitation for participants to settle in before starting the class.
- The speaker, Dr. Filiaga Armiquedías, confirms that she can be heard and prepares to start the class after a brief wait.
Presentation of the Topic
- Dr. Filiaga introduces herself as a geriatrician from the naval hospital and outlines that today's topic will focus on diabetes from a unique perspective, emphasizing understanding the individual rather than just numerical data.
- She highlights that managing diabetes in older adults requires consideration of five domains: functionality, cognition, social aspects, nutrition, and emotional health.
Understanding Diabetes Management
Key Concepts in Geriatric Diabetes Care
- The central message is that clinical criteria for diabetes management extend beyond laboratory numbers; they must consider the patient's overall context.
- Dr. Filiaga engages participants by asking how many have encountered elderly patients with diabetes during their clinical practices.
Participant Engagement
- A participant shares experiences seeing many elderly patients with diabetes and questions whether all should have uniform glucose targets.
- Discussion arises about whether treatment goals should vary based on patient functionality and robustness.
Epidemiology of Diabetes in Older Adults
Prevalence Insights
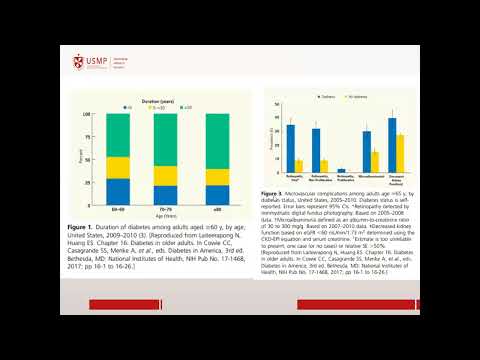
- More than 90% of older adults with diabetes have type 2 diabetes; nearly half over 65 are pre-diabetic.
- Incidence rates increase significantly among those aged 65 to 79 years, indicating a growing concern for this demographic.
Implications of Aging on Diabetes
- As life expectancy increases (with some living past 90), more individuals will live longer with chronic conditions like diabetes.
Factors Influencing Diabetes Prevalence
Age-related Changes
- Aging leads to physiological changes such as increased fibrosis and decreased pancreatic function, contributing to higher incidence rates of type 2 diabetes.
External Factors Impacting Health
- Discussion includes intrinsic factors (like aging physiology affecting insulin secretion) versus extrinsic factors (such as obesity, sedentary lifestyle, diet), highlighting their roles in increasing diabetes prevalence among older adults.
Impact of Aging on Diabetes Management
Metabolic Syndrome and Complications in Older Adults
- The prevalence of metabolic syndrome is significant among older adults, impacting their health outcomes.
- Diabetes complications such as diabetic polyneuropathy and retinopathy are common, leading to increased morbidity.
Late Manifestations of Diabetes
- Hospitalized patients often present with late manifestations of diabetes, including neuropathy, nephropathy, and retinopathy. These conditions severely affect quality of life.
- The presence of these complications can lead to a loss of independence and autonomy for older adults living with diabetes.
Geriatric Considerations in Diabetes Management
- Differentiating between frail older adults and those with good support systems is crucial for effective diabetes management. Treatment approaches must be tailored accordingly.
- Comprehensive geriatric assessment should include evaluating glucose levels alongside assessing functional status and frailty indicators. This holistic approach informs treatment plans.
Individualized Treatment Goals
- Treatment goals vary significantly based on the patient's overall health status; robust patients may aim for normal glucose levels while frail individuals may prioritize avoiding hypoglycemia over strict glycemic control.
- In cases where patients have high glucose levels but lack family support or regular medication adherence, the focus shifts from achieving ideal glycemic targets to preventing severe complications like hypoglycemia.
Challenges in Managing Insulin Resistance
- Aging exacerbates insulin resistance and alters beta-cell function, complicating diabetes management in older adults who often have reduced metabolic reserves due to muscle loss and increased visceral fat accumulation.
- Fragile elderly patients are more susceptible to rapid decompensation during acute illnesses or infections, making standard treatment protocols less applicable for this demographic group.
Therapeutic Errors in Elderly Care
- Applying standard treatment regimens without considering individual patient fragility can lead to therapeutic errors that worsen patient outcomes, particularly regarding hypoglycemia risks in vulnerable populations.
- Understanding the unique physiological responses of older adults is essential for tailoring interventions that minimize adverse effects while managing diabetes effectively.
Understanding Sarcopenia and Its Impact on Glycemic Control
Functional Reserve and Metabolic Changes
- The reduction in functional reserve and metabolic capacity, along with increased visceral fat, alters glucose control in older adults. This necessitates adjustments in treatment parameters based on the specific group being addressed.
Sarcopenia's Role in Older Adults
- Sarcopenia, characterized by muscle mass loss and fatigue, negatively impacts glycemic control in older adults. A good muscle reserve is essential for effective glucose management; thus, sarcopenia exacerbates challenges in this area.
Compounding Factors Affecting Health
- The combination of aging, polypharmacy (multiple medications), sarcopenia, and infections increases fragility among older adults. This raises concerns about maintaining metabolic reserves necessary for health management.
Treatment Considerations
- Historical approaches to insulin administration did not account for age or patient fragility, leading to potential hypoglycemia due to generalized treatment protocols that failed to consider individual functional status. Adjustments are now needed based on comprehensive assessments of patients' conditions rather than solely their weight or glucose levels.
Importance of Individualized Assessment
- It is crucial to evaluate each patient's functionality and social environment when determining treatment plans for diabetes management in older adults. This individualized approach helps avoid stigmatization based on age alone while ensuring appropriate care strategies are implemented.
Screening for Diabetes in Older Adults
Prevalence of Diabetes Among Seniors
- Many older adults may be undiagnosed with diabetes despite presenting without symptoms; therefore, proactive screening is essential as physiological changes increase their risk for diabetes complications over time.
Recommended Screening Practices
- Regular testing such as fasting blood glucose and hemoglobin A1C should be part of the geriatric profile to identify diabetes or prediabetes early enough to prevent severe complications like neuropathy or cognitive decline that significantly affect quality of life.
Age Considerations for Prevention
- There is no strict upper age limit beyond which diabetes prevention efforts should cease; even elderly individuals can benefit from diagnosis and management interventions due to the insidious nature of diabetic symptoms that can lead to serious health issues if left untreated.
Understanding Diabetes Management in Older Adults
Importance of Age and Context in Diabetes Diagnosis
- Age is a significant factor, but context and individual health dimensions are crucial for understanding diabetes management. For instance, patients over 80 may present unique challenges such as pre-frailty or early diabetes diagnosis.
Defining Prediabetes and Diabetes
- Prediabetes is identified when fasting glucose levels exceed 100 mg/dL, while established diabetes is diagnosed at levels above 126 mg/dL fasting or greater than 200 mg/dL postprandial. Hemoglobin A1c values above 6.5% also indicate diabetes. These benchmarks are essential for accurate diagnosis.
Treatment Considerations for Older Adults
- Treatment strategies must adapt based on the patient's overall health status and expectations. Evaluating general health, functional abilities, cognitive status, BMI, hypertension history, substance use (tobacco/alcohol), cancer history, and current medications is vital for tailoring treatment plans.
Cognitive Assessment in Elderly Patients
- Regular cognitive assessments are recommended for patients over 65 to detect any decline that could complicate diabetes management. Cognitive impairment can hinder a patient’s ability to follow complex treatment regimens effectively.
Risks Associated with Complex Treatment Regimens
- Patients with uncontrolled dementia face significant risks when managing diabetes due to potential misunderstandings about medication dosages or dietary needs leading to hypoglycemia or other complications. Simplifying treatment plans may be necessary to ensure safety and adherence among these patients.
Understanding Diabetes Management in Older Adults
Importance of Simplifying Treatment Approaches
- The complexity of diabetes management can lead to biases in treatment, especially when multiple pathologies are involved. It's crucial to avoid overly complicated schemes that may not be effective.
Geriatric Treatment Principles
- In geriatrics, the primary focus should not solely be on treating hyperglycemia but also on preventing hypoglycemia, which poses significant risks for older adults.
Risks Associated with Hypoglycemia
- Preventing hypoglycemia is vital as it can lead to severe consequences such as fainting and falls, which may result in fractures and subsequent hospitalizations.
- Hospitalization increases the risk of complications like infections and delirium, further deteriorating the health of older patients.
Comprehensive Geriatric Assessment (CGA)
- A tailored treatment plan must consider a comprehensive geriatric assessment (CGA), evaluating functionality, cognitive status, family support, and nutritional health.
- Effective diabetes management includes reducing hypoglycemia risk while controlling blood sugar levels through lifestyle modifications.
Lifestyle Modifications as First-Line Treatment
- For older adults with hyperglycemia, lifestyle changes should be prioritized over pharmacological treatments. This includes promoting physical activity and proper hydration.
- Even patients with dementia can benefit from structured activities that enhance their quality of life without immediately resorting to medications.
Monitoring and Nutritional Assessment
- Regular monitoring is essential; however, it should be balanced to avoid unnecessary discomfort from frequent glucose testing.
- Pharmacological interventions must be carefully supervised based on individual patient assessments rather than defaulting to medication as first-line therapy.
- Evaluating nutritional status using standardized scales is critical for developing effective care plans for older adults with diabetes.
Nutritional Assessment and Management in Older Adults with Diabetes
Importance of Nutritional Assessment
- The focus is on validating malnutrition and monitoring progress over time. The Nutritional Assessment (MNNA) scale is emphasized for evaluating nutritional risk, particularly in patients over 65 with diabetes and frailty.
- It is crucial to implement dietary changes gradually rather than imposing strict restrictions, as excessive limitations can lead to more severe malnutrition than high glucose levels.
Dietary Considerations
- Emphasizing the importance of protein intake for older adults unless contraindicated by renal issues; adequate caloric intake is also vital for preventing malnutrition.
- The MNNA scale is validated for use in the Peruvian population, highlighting that nutrition not only improves glucose levels but also protects overall functionality in older adults.
Pharmacological Therapy
- A stepwise approach to pharmacological therapy is recommended, starting with metformin if there are no contraindications; treatment must be individualized based on patient tolerance and specific conditions.
- Complications such as nephropathy, cardiopathy, retinopathy, and neuropathy are significant concerns in geriatrics due to their impact on functionality; many patients may have undiagnosed diabetes for years prior to diagnosis.
Managing Complications
- Collaborative management involving ophthalmologists, cardiologists, neurologists, and nephrologists is essential to address microvascular complications effectively. Understanding these interrelations helps manage risks like heart failure better.
- Neuropathy can lead to instability and increased fall risk due to altered sensitivity; addressing this through physical rehabilitation becomes critical in managing diabetic complications effectively.
Preventing Falls and Foot Care
- Recognizing the role of diabetic neuropathy in increasing fall risk emphasizes the need for a multidisciplinary approach including physiotherapy and podiatry care; proper footwear assessment is crucial.
- Chronic kidney disease impacts treatment options significantly; understanding glomerular filtration rates helps determine appropriate medications while avoiding those that could exacerbate renal issues when GFR falls below 30 mL/min.
Understanding Renal Function in Diabetes Management
Importance of Renal Function Assessment
- The assessment of renal function is crucial as it guides treatment adjustments and helps avoid nephrotoxic medications. This ensures that the patient's renal function does not deteriorate further, especially in diabetic patients who may have multiple comorbidities.
Holistic Approach to Elderly Diabetes Care
- Managing diabetes in older adults involves more than just laboratory measurements; it requires ensuring a good quality of life, memory retention, and decision-making capabilities. Geriatrics focuses on treating individuals holistically rather than merely addressing their diseases or organ functions.
Centrality of the Patient in Geriatric Care
- Geriatrics emphasizes treating the elderly as whole persons rather than focusing solely on their medical conditions. It is essential to consider their functionality and personal choices when planning treatments to maintain their quality of life.
Parameters for Diabetes Management in Older Adults
Adjusting Treatment Parameters
- In older adults with functional dependence, standard parameters for glucose management may not apply. The focus shifts from maintaining strict glucose levels to preventing hypoglycemia while managing overall health outcomes effectively.
Prioritizing Symptom Management
- For patients nearing end-of-life stages, the priority changes from controlling blood sugar levels to alleviating symptoms and enhancing comfort, indicating a shift in treatment goals based on patient needs and circumstances.
Diabetes Diagnosis Criteria for Older Adults
Reference Values for HbA1c Levels
- Different groups within the elderly population require tailored reference values for hemoglobin A1c (HbA1c) based on their health status and comorbidities, emphasizing individualized care approaches depending on functional capacity and chronic disease burden.
Classification Based on Functional Status
- Elderly patients can be classified into groups based on their number of chronic illnesses and functional independence, which influences target glucose levels—aiming for less stringent control in those with significant dependencies or terminal conditions.
Understanding Medication Challenges in Patients with Swallowing Disorders
The Issue of Medication Administration
- A question arises regarding the administration of metformin for diabetic patients experiencing swallowing difficulties. The size of the metformin tablet poses a challenge, as it cannot be easily crushed without losing its efficacy.
- Alternative medications like GLP-1 agonists are discussed as they offer different dosages and potentially lower risks of hypoglycemia, emphasizing the need for careful monitoring based on individual patient needs.
Managing Advanced Dementia and Swallowing Disorders
- In cases of advanced dementia, managing feeding becomes crucial. Lifestyle changes and dietary adjustments are highlighted as primary strategies to address these challenges effectively.
- The discussion emphasizes weighing the risks and benefits of using hypoglycemic agents in patients with swallowing disorders. There is concern that focusing solely on administering metformin may overlook broader dietary issues affecting overall health.
Diagnostic Considerations
- A query about ultrasound tests leads to clarification that such imaging is used to rule out abdominal aortic aneurysms, underscoring the importance of thorough diagnostic evaluations in managing complex medical conditions.
Conclusion
- The session concludes with an invitation for further questions, indicating openness to continued dialogue and support among participants regarding patient care challenges.