CLASE TEÓRICA 6 - INFLAMACIÓN Y REPARACIÓN TISULAR PARTE 1
Inflammation: Generalities and Repair
Introduction to Inflammation
- Ismael Fonseca introduces the topic of inflammation, defining it as a reaction of vascularized living tissues in response to local aggression.
- Emphasizes that inflammation requires vascularization; without blood vessels, inflammation cannot occur.
Types of Inflammation
- Discusses two types of inflammatory responses: acute (rapid onset) and chronic (slow development), depending on the nature of the stimulus and the organism's ability to eliminate it.
- Acute inflammation can lead to resolution, organization (formation of granulation tissue), abscess formation, or healing/restoration.
Chronic Inflammation
- Chronic inflammation may arise from persistent infections or prolonged exposure to toxic agents, both exogenous and endogenous.
- Autoimmune diseases are highlighted as conditions where antibodies attack the body's own tissues due to loss of tolerance.
Cardinal Signs of Inflammation
- Local phenomena include cardinal signs known as "the four humors" by Celsus: swelling (tumor), redness (rubor), heat (calor), and pain (dolor).
- A fifth sign, loss of function, is introduced; for example, arthritis can limit joint movement.
Mechanisms of Acute Inflammation
- Acute inflammation serves as a rapid host response aimed at neutralizing harmful agents through three essential components:
- Vascular caliber alterations increase blood flow at injury sites.
- Structural changes in microcirculation allow plasma proteins and leukocytes to exit circulation.
- Leukocyte migration accumulates at injury sites for elimination purposes.
Events in Microcirculation During Inflammation
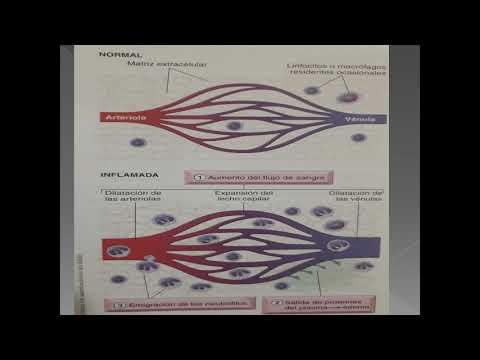
- Key events during acute inflammatory processes include vasodilation leading to increased blood flow due to stasis—an abnormal slowing down in circulation.
- The process involves marginating blood elements followed by rolling, adhesion, and eventual migration through vessel walls.
Exudate vs. Transudate Formation
- A comparative overview is provided regarding normal circulation versus manifestations during acute inflammation.
Inflammatory Processes and Cellular Responses
Mechanisms of Exudate Formation
- The formation of exudate during inflammation is due to increased vascular permeability, mediated by chemical mediators such as histamine.
- This increase in permeability results from the widening of inter-endothelial spaces, allowing fluid and proteins to escape into surrounding tissues.
Role of Blood Components in Inflammation
- Various blood components, including connective tissue cells like mast cells, play a crucial role in acute inflammatory responses. Mast cells release granules rich in serotonin during inflammation.
- Fibroblasts are also significant for wound repair, while macrophages perform phagocytosis through a three-step process: recognition, engulfment, and destruction of foreign agents.
Extracellular Matrix Contributions
- Elements of the extracellular matrix (ECM), such as elastic fibers, collagen fibers, and proteoglycans, contribute to the structural changes observed during acute inflammation.
Leukocyte Margination Process
- The margination process involves leukocytes moving from central circulation towards the vessel wall due to changes in blood flow dynamics (stasis). This is followed by rolling along the vascular endothelium.
- Key molecules involved include selectins for rolling and integrins for adhesion; CD31 facilitates migration through opened endothelial junctions.
Histological Changes During Inflammation
- In lung tissue affected by acute inflammation, alveolar septa thicken due to vasodilation; dilated vessels can be observed alongside an influx of immune cells like neutrophils at the site of injury.
- The first responders in acute inflammation are polymorphonuclear leukocytes (neutrophils), which dominate early stages before transitioning to mononuclear cell involvement in chronic cases.
Evolution of Inflammatory Response
- Acute inflammation may resolve completely or progress towards abscess formation or chronicity characterized by angiogenesis and a shift from neutrophilic infiltration to mononuclear cell predominance.
Inflammatory Processes and Exudates
Histological Changes in Chronic Inflammation
- The transcript discusses the interruption of cell flow to inflammation sites, highlighting histological changes associated with chronic inflammatory processes. Dense inflammatory infiltrates are observed, particularly composed of lymphocytes and monocytes.
- The presence of cuboidal cells in pulmonary tissue is noted, along with the development of connective tissue marked by arrows, indicating a transition from loose connective tissue to fibrosis over time.
Types of Exudates
- An exudate is defined as an inflammatory fluid rich in cells and proteins, with a density greater than 1020. This contrasts with transudate, which has fewer cells and proteins and a lower density.
- Different types of exudates are identified: catarrhal (seen in upper respiratory conditions), serous, fibrinous, hemorrhagic, and pseudomembranous (as seen in pseudomembranous colitis caused by Clostridium).
Examples of Exudates
- Serous exudate is characterized by clear or translucent liquid accumulation from plasma or mesothelial cell secretion. This can be observed in skin lesions like blisters.
- Fibrinous exudate is illustrated through images showing white plaques on the pericardium during conditions like rheumatic fever that cause pancarditis (inflammation of all heart layers).
Characteristics of Fibrinous Exudate
- Fibrinous exudate contains high levels of fibrin protein; macroscopically it appears as whitish plaques. Histologically, it shows acidophilic material deposits alongside moderate inflammatory infiltrates.
Hemorrhagic Exudate Insights
- Hemorrhagic exudate relates to chronic destructive processes such as tuberculosis or disseminated cancer. It differs from true hemorrhage since it consists mainly of blood due to underlying pathological conditions rather than vascular rupture.